Constipation Isn't Normal: Root Causes, Natural Fixes, and Why Fiber Isn't Always the Answer
Apr 29, 2026
Going a few times a week, relying on coffee to kickstart your digestion, or ending every day feeling bloated and backed up are experiences far more common than most people talk about. And yet, common does not mean normal.
Constipation is one of the most frequently dismissed digestive complaints in practice. People are told to drink more water, eat more fiber, and move on. Sometimes those suggestions help temporarily. More often, nothing meaningfully changes, and the symptom becomes something people quietly learn to manage rather than something they expect to resolve.
Constipation is rarely a single-cause problem, and it almost never comes down to fiber alone. When it persists, the body is usually signaling that something deeper needs attention.
Constipation Symptoms That Often Go Unrecognized
Constipation does not always present the way most people picture it. It can show up differently from person to person, which is part of why it goes unaddressed for so long. Symptoms can include:
- Fewer than one bowel movement per day
- Stools that are hard, dry, or difficult to pass
- A persistent feeling of incomplete evacuation
- Bloating or abdominal pressure throughout the day
- Reliance on coffee, magnesium, or laxatives to go
- Sluggish digestion, low appetite, or feeling full quickly
- Fatigue or skin issues running alongside digestive symptoms
Many of these overlap with sluggish motility, gut imbalance, and digestive dysfunction which points to something more systemic than a simple lack of fiber.
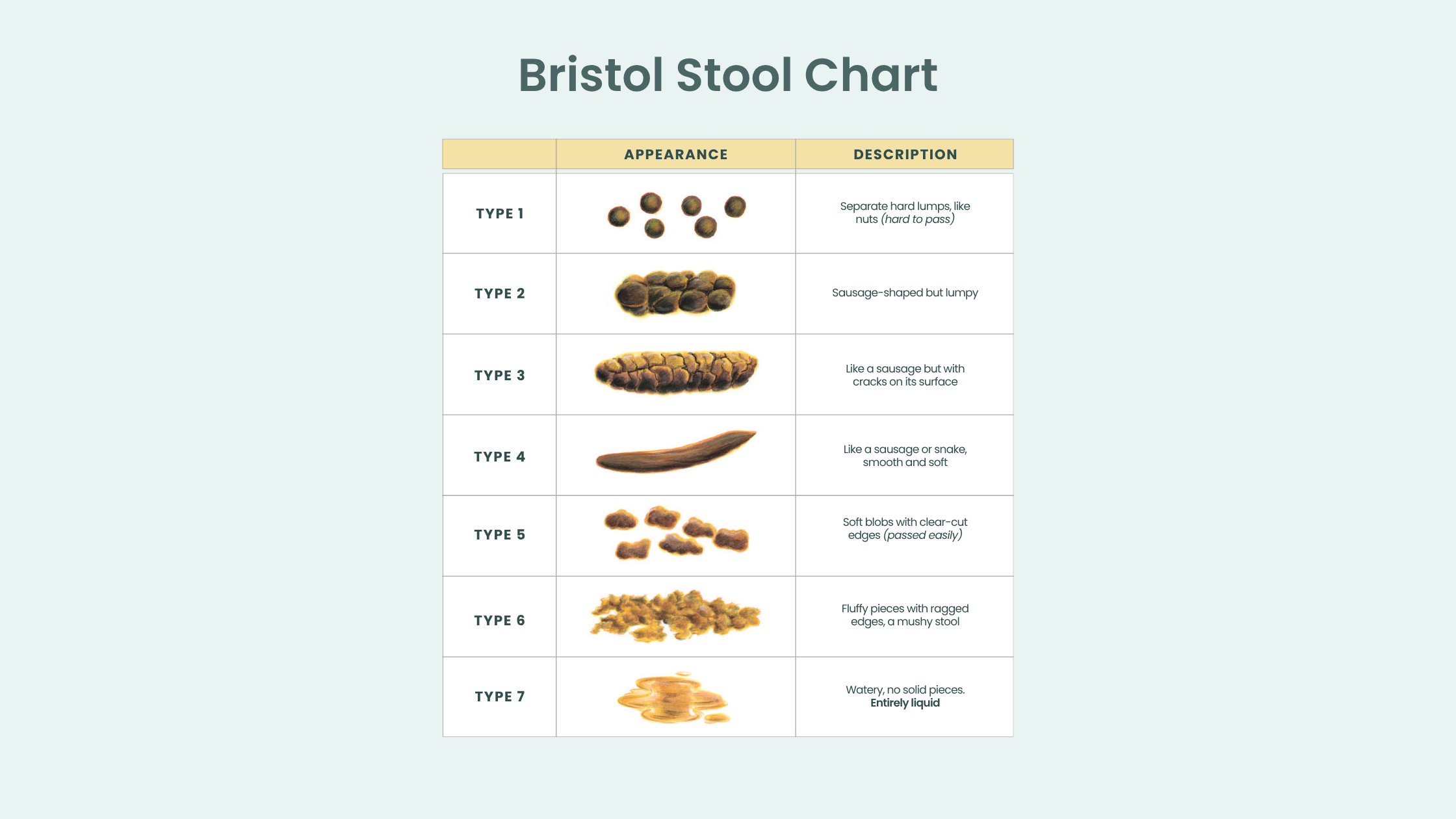
The Bristol Stool Chart is a useful clinical reference for understanding stool consistency. Types 1 and 2 on the chart are the recognized indicators of constipation, characterized as hard, lumpy stools that are difficult to pass.
What Causes Constipation?
The frustrating part about constipation is that it tends to have more than one thing behind it. Most people spend a long time treating the symptom without ever understanding what the body is actually responding to. These are the most common contributors:
Stress and the Nervous System
The gut operates primarily in a parasympathetic state, often called "rest and digest." When the body is under chronic stress, it spends more time in a sympathetic, high-alert state and digestion suffers as a result. Stress can reduce gut motility, decrease digestive secretions, and disrupt the signaling between the brain and the gut. This is why constipation tends to worsen during demanding seasons of life and improve when the nervous system finally gets a chance to settle.
Hormonal Imbalances
Hormones have a more direct influence on bowel function than most people realize. Progesterone, which rises in the second half of the menstrual cycle, has a relaxing effect on smooth muscle throughout the digestive tract and can slow motility significantly. Thyroid imbalances are also strongly associated with constipation. Elevated cortisol from ongoing stress adds another layer of disruption. For many people, noticing a consistent pattern of constipation at certain points in their cycle or during high-stress periods is one of the first clues that hormones are part of the picture.
Low Bile Flow
Bile does more than support fat digestion. It also plays a huge role in stimulating bowel movements and keeping stool at the right consistency. When bile flow is sluggish, stools can become dry and hard, motility slows, and fat digestion may feel off. Low bile output is often connected to diet and liver function, and it is one of the most overlooked contributors to chronic constipation.
Gut Microbiome Imbalance
The gut microbiome has a significant influence on how well the digestive tract moves. Beneficial bacteria produce short-chain fatty acids, compounds that support gut motility and nourish the cells lining the intestinal wall. When microbial balance is disrupted, short-chain fatty acid production drops and transit time slows. Studies show that people with functional constipation tend to have reduced levels of beneficial bacteria like Lactobacillus and Bifidobacterium, alongside a relative increase in opportunistic strains. Further research confirms that reduced short-chain fatty acid levels impair intestinal motility and promote inflammation, while altered bile acid metabolism disrupts the receptor-mediated signaling that affects gut transit.
Why Fiber Alone Is Not Enough
Many people have tried drinking more water, adding fiber, cutting trigger foods, and taking a probiotic, and the results are inconsistent at best.
Constipation is a function problem, not a fiber problem. When gut motility is already sluggish, adding more fiber can worsen things by increasing bulk without improving movement. Fiber is most effective when the gut environment is already functioning well enough to move it through. Without understanding why digestion has slowed, continuing to add the same strategies becomes a cycle of temporary relief and returning symptoms.
How Functional Gut Testing Helps Identify the Root Cause of Constipation
For people who have been managing constipation for months or years without resolution, comprehensive stool testing can offer a level of clarity that symptoms alone cannot. A functional stool test examines digestion and absorption markers, inflammation patterns, and microbial balance, providing a direct picture of what is contributing to sluggish gut function.
For constipation specifically, testing can help identify whether motility issues are connected to microbial patterns, whether inflammation is playing a role, and whether digestive support like bile or enzymes may be warranted. It does not replace nutrition and lifestyle work. It makes that work more targeted and far more likely to produce lasting results.
Treating Constipation at the Root
Once the contributing patterns are better understood, the approach to healing becomes much more intentional. Rather than layering on supplements or removing more foods, a root-cause plan builds the conditions the gut needs to function well on its own.
- Targeted nutrition
Focuses on balanced meals with adequate protein, fat, and strategic fiber. The goal is to feed beneficial bacteria and support motility without overwhelming a sluggish system. Hydration matters too, particularly the timing and quality of fluids relative to meals. - Digestive support
May include magnesium for motility and bitter foods or herbs to stimulate bile flow. Gentle support for stomach acid and enzyme production is also considered when indicated by testing or clinical patterns. - Nervous system regulation
Addresses the gut-brain connection directly. Slowing down while eating, supporting sleep, building daily rhythm, and working through chronic stress patterns all have a measurable effect on how well the gut moves. - Microbiome support
Focuses on increasing microbial diversity through prebiotic and probiotic foods and addressing specific imbalances when identified. Supporting the production of short-chain fatty acids is a central part of restoring motility from the inside out.
The goal throughout is to help the body restore its own function, building toward a gut that works well without ongoing dependency on supplements or laxatives.
Next Steps
We work with people who are tired of managing constipation as a fact of life and want a plan that addresses what is driving it. Through personalized nutrition, functional testing when appropriate, and education at every step, the focus is on building a sustainable path toward a gut that works.
Start with the free Gut Health Assessment to identify patterns that may be contributing to your symptoms, or explore the Gut Restore Assessment for a comprehensive evaluation that includes stool testing and a personalized results review. You can also schedule a free discovery call to talk through your situation directly.
Frequently Asked Questions
Is constipation a sign of poor gut health?
It can be. Constipation is often a signal that gut motility, microbial balance, or digestive function needs support, and addressing those patterns tends to be more effective than treating the symptom on its own.
Can stress cause constipation?
Yes. Chronic stress shifts the body away from its rest-and-digest state, which slows motility and disrupts normal signaling between the brain and gut. For many people, stress is one of the primary drivers of ongoing constipation.
Can hormones affect bowel movements?
Significantly. Rising progesterone in the second half of the menstrual cycle can slow motility, thyroid imbalances are strongly linked to constipation, and elevated cortisol from chronic stress disrupts digestive function. Tracking patterns across the cycle is often a helpful starting point.
What does low bile have to do with constipation?
Bile helps stimulate bowel movements and maintain stool consistency. When bile flow is sluggish, stools can become dry and hard and overall motility slows. Supporting liver and digestive function is often a meaningful piece of the puzzle for people with chronic constipation.
Can constipation affect more than just digestion?
It can. Chronic constipation is often accompanied by fatigue, skin issues, brain fog, and a general sense of feeling off. When waste is not moving through efficiently, the effects tend to show up beyond the gut.
How long does it take to see improvement with a root-cause approach?
It varies depending on the underlying cause and how long symptoms have been present. Most people begin to notice meaningful changes within a few weeks to a few months when working with a targeted, personalized plan.
Is stool testing helpful for constipation?
For people with persistent constipation who have not found answers through standard approaches, functional stool testing can provide valuable insight into microbial balance, inflammation, and digestion patterns, helping guide a more personalized approach to gut healing.
DON’T MISS THIS!
START YOUR PATH TO BETTER HEALTH
Take our free Gut Health Assessment today and discover personalized steps to improve your digestion and well-being. Don’t wait—unlock the key to a healthier you now!


